No More Federal Dollars for Residency Positions
Annual graduates continue to increase at rates must faster than population growth or growth of the elderly, yet more sources all expanded have failed to address shortages. Where did the graduates go? Not surprisingly they follow the dollar directions shaped by health policy. GME training produces the wrong physicians for the wrong specialties and the wrong places.
Residency expansions could increase the physician workforce but will not address shortages of workforce, poor retention of graduates where needed, health outcomes improvements, or access to care for Medicaid and Medicare populations falling most behind. Residency expansions will worsen health care costs and will further marginalize physicians in their contracts with employers. New medical schools, residency programs, or nurse practitioner/physician assistant programs should not be promoted as a solution for health access woes. Only substantially more dollars to support more team members in lowest concentration settings will address health access deficits.
Graduate Expansions Fail for Relief of Shortages
Graduate Expansions Fail for Relief of Shortages
- Residency expansions cannot address shortages. Too few dollars go to the places to allow adequate team members. Only payment changes can address shortages.
- Residency expansions cannot address poor retention and higher turnover where payments are least, support is least, and complexity is highest. Only payment changes can address these areas.
- Residency training continues to produce the wrong specialties for the wrong places. The payment design prevents MD DO NP and PA from remaining within primary care careers and prevents residency graduates from staying within general specialties as taking a fellowship or two results in a great deal more support with less complexity and more team members to share the load.
- Uses of Medicare and Medicaid dollars for training are not specific to the needs of Medicare and Medicaid patients most left behind. The designs prevent graduates from going to places where such patients are concentrated and prevent the specialties that they most need.
Health Care Cost Acceleration
Expansions of residency positions are promoted by those who most benefit from such expansions. Fewer graduates can help to prevent runaway health care costs. Nurse practitioners and physician assistants have long been promoted as excellent contributions for primary care, but do as well or better in subspecialty teams. More patients can be seen in more settings and the physicians can focus on the highest revenue areas.
Accelerations of health care costs are a primary mechanism resulting in across the board cuts - cuts that hurt the lowest margin practices. The lowest margins are seen in generalist and general specialty workforce.
Overproduction
Too many MD DO NP and PA graduates are being produced. The growth far outstrips population growth and growth of the elderly. The result has been employer dominated workforce. This tips the balance greatly toward employers, particularly in areas with the least payment support. Various sources are played against one another and this prevents understanding of the damage done by too many graduates.
Inequities Contribute to Disparities and Poor Outcomes
Residency funding is distributed most inequitably, adding to disparities directly in dollar distributions with further contributions in the products produced. Only 6.5% of residency positions are found in lowest physician concentration counties with 40% of Americans and 43 - 47% of the elderly, poor, and others most left behind.
Residency
training design is a great fit for the highest physician concentration places. These include 6
states, 100 counties, and 1100 zip codes that already have top
concentrations of physicians.
Residency is the dominant factor in practice location. About half of residency positions and 45% of physicians are found in 1% of the land area in 1100
zip codes that have the most lines of revenue and the highest
reimbursements in each line. These are crafted by payment designs that leaders in top concentrations have largely
shaped and protected.
Research
has long established that physicians will crowd in to higher
concentration places rather than to distribute to places of need.
Too Many Graduates Already
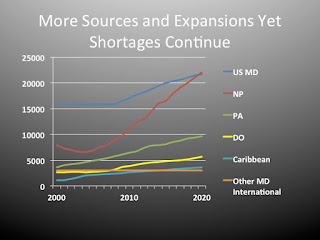
By the end of 1980 the US had 20000 physicians entering the workforce with 1500 for PA and 1500 for NP. Now 30,000 physicians enter the workforce with 20,000 for NP and 9000 for PA. In only a few years there will be more NP and PA than physicians. Each year brings a few thousand more NP graduates with no sign of slowing. New medical schools are being added and new PA programs as well.
The US will never resolve shortages by producing more graduates. Massive expansions have long failed as demonstrated with a 12 times increase in nurse practitioners since 1980 along with a 6 times increase in PA and two doublings of DO graduates plus 25% from international sources plus a 30% increase in MD graduates.
These
increases have resulted in little or no increase in primary care and a
massive increase in non-primary care workforce.
Health care institutions, corporations, and businesses prefer to
generate more revenue from services, tests, procedures, and evaluations
that are paid at much higher rates. It is even better if this has lower overhead. Primary care and basic services are high in overhead and low in revenue. Businesses invest where profit is most likely and payment designs have take away the profit in primary care for decades.
Expansions Fail for Primary Care, Mental Health, and General Surgical Specialties
Despite
recent expansions, the collapse of internal medicine primary care,
family medicine down to 70% primary care result, and pediatrics down
below 40% have resulted in less physician primary care. Each year the US
gets less primary care result despite more graduates.
The
last doublings of physician assistant and osteopathic graduates
resulted in no net gain in primary care workforce. The entire expansion
was devoted to non-primary care.
The last few decades of workforce expansion have entirely been in non-primary care highly specialized workforce areas in places with higher concentrations of workforce - where we already overutilize and have costs too high. Too Many and the Wrong Clinicians. The dollars expended follow the workforce to more spent for procedural, technical, hospital, and highly subspecialized leaving less for primary care and basic services.
Primary care spending and spending where people need care has remained stagnant for decades by design. NP and PA also add more specialties and more are added to each new specialty - leaving family practice positions behind - the predominant primary care form for NP PA and DO.
Even family medicine is no longer immune to payment paucity with over 90% active in FM dropping to less than 70% in the last 15 class years. Family medicine may soon break the 50% mark with less than a majority remaining active and in primary care over their careers. This could begin in the next few class years due to insufficient primary care support, costly complications, and rapid increases in complexity. Burnout is at record high levels due to payment design.
Primary care turnover costs are estimated to be over $300,000 per lost primary care physician or about twice the cost of loss of NP and PA clinicians, but clinicians turn over at twice the rate of primary care physicians. Worsening morale, productivity, burnout, and turnover result in negative margins.
Flexible workforce follows funding. Once primary care training physicians had no other options, but now they have many hospital, urgent, emergent, and specialty options. NP and PA graduates once had few options, but this is no longer the case. As with physicians, they have more support and more team members and more specialized roles with less complexity and higher salaries - all set up by payment design.
Flexible workforce follows funding. Once primary care training physicians had no other options, but now they have many hospital, urgent, emergent, and specialty options. NP and PA graduates once had few options, but this is no longer the case. As with physicians, they have more support and more team members and more specialized roles with less complexity and higher salaries - all set up by payment design.
The Evidence All Points to Payment Failure
The evidence points to shortages as the result of payment design. Only the academic community clings to workforce as being shaped by training. Without the dollars injected into the services provided by basic specialties, there can be no resolution of shortages.
The nation needs generalists, mental health, and general surgical specialties now and for decades to come due to aging changes. This is even more important where most Americans are found with lowest concentrations of workforce as there are few other types of specialties.
These basic services are lowest paid services and remain so by design. The MD DO NP and PA expansions do not reflect any movement toward addressing these workforce areas because of payment design. The failure of massive expansions should have long ago pointed to payment failure.
These basic services are lowest paid services and remain so by design. The MD DO NP and PA expansions do not reflect any movement toward addressing these workforce areas because of payment design. The failure of massive expansions should have long ago pointed to payment failure.
Payment Failure Fails Most Where Workforce is Most Needed.
Demand increases are greatest in 2621 lowest physician concentration counties that are growing the fastest
- In population (30% faster for decades)
- In elderly
- In chronic diseases
- In complexity
Americans in higher concentrations are being displaced by city, county, developer, and government designs. Land is most valuable in higher concentration settings. Converting areas of lowest value (affordable housing, older housing, public housing) to highest value is quite profitable. Many participate in these schemes. Articles indicate the worsening shortages of affordable housing across metro areas of the nation.
Destruction of affordable housing in higher concentration settings forces Americans who are older, less healthy, disabled, Veterans, Medicare, Medicaid, and Dual Eligible to go to lowest concentration counties - counties with the least resources and workforce. They bring their worst paying, least locally supportive insurance plans with them. These plans now exclude local providers, often pay less than cost of delivery, and require numerous hoops to jump through to address patient and payer needs. Those who do not want to take care of them include state, federal, and insurance payers. Providers caring for them get penalized by payment design because they care for them.
Concentrations of Patients with Lowest Paying Plans Shape Shortages of Workforce
The lowest concentration counties are shortest in workforce with 40% of the population and less than 13% of health spending. Only 22 - 26% of physicians, clinicians, internists, pediatricians, and general surgical specialties are found in this 40% segment.
In these counties about 46% of local workforce is primary care and 25% are found in general surgical specialties. Practices in these counties tend to have the oldest physicians - also an indication of lack of replacement. These counties have been hit hardest by recent designs that have compromised small practices - particularly the MD DO NP and PA that remain in family practice despite the design.
In these counties about 46% of local workforce is primary care and 25% are found in general surgical specialties. Practices in these counties tend to have the oldest physicians - also an indication of lack of replacement. These counties have been hit hardest by recent designs that have compromised small practices - particularly the MD DO NP and PA that remain in family practice despite the design.
The specialties important for lowest concentration counties are in decline or are disappearing. In the following graphic the ratio of concentration is noted, followed by active physicians per 100,000, the proportion of the local workforce provided by the specialty, and expected changes.
Family medicine distributes most equitably at 1.18. Psychiatrists are 7 times more likely to be found in the 79 top physician concentration counties as compared to the 2621 lowest physician concentration counties. Family medicine remains at 26 to 32 active family physicians per 100,000 across the US and various divisions. In the very lowest concentration counties, only family practice is found. In top concentrations FM is only 3 - 5% of local workforce. Where policies are most shaped, family medicine is a small fraction. Where health access is most important, family medicine most matters. Family practice NP and PA have similar distribution, but only when staying in family practice positions.
Only the general specialties provide much care in lowest concentration counties
and only when they stay general and do not go on for one or more fellowships.
Note that residents are 150 per 100,000 in the 79 top concentration counties - a level much higher than 115 active physicians per 100,000 from all specialties as found in the 2621 lowest physician concentration counties. It is a great advantage to design a new line of revenue specific to higher concentration settings.
General specialties are in decline and some are collapsing. In recent years, new specialties have replaced old as seen in pulmonary, oncology, and radiology. The new forms of oncology and pulmonary critical care and radiology do not distribute well at all and are replacing the older more general types. This is a reflection of differences in training and lack of distribution of those younger.
Hospital closures are predominantly in these lowest concentration counties and the closures force the departure of 20 - 30% of local workforce. Care of challenging populations with lesser health results in more penalties - a known consequence of Pay for Performance.
The loss of a hospital also forces delays in the care of urgent and emergent care needs such as involving trauma, falls, sepsis, acute vascular events, respiratory failure, asthma, allergic reactions, dehydration, burns, and other conditions.There are more ways for children, infants, new mothers, pregnant women, toddlers, teens, and older Americans to die - by design.
Hospital closures are predominantly in these lowest concentration counties and the closures force the departure of 20 - 30% of local workforce. Care of challenging populations with lesser health results in more penalties - a known consequence of Pay for Performance.
The loss of a hospital also forces delays in the care of urgent and emergent care needs such as involving trauma, falls, sepsis, acute vascular events, respiratory failure, asthma, allergic reactions, dehydration, burns, and other conditions.There are more ways for children, infants, new mothers, pregnant women, toddlers, teens, and older Americans to die - by design.
Poor Fit All Around
Resident training depends upon medical school selections. Medical schools select the wrong origins for these careers and locations. Medical schools train wrong for these careers and locations. An initial residency is just a stepping stone past these careers and locations. Payment design prevents these careers and locations.
Just one fellowship that greatly benefits the teaching hospital allows the residency graduate to bypass what is needed to a place with better support, more team members, and less complexity along with higher salary and opportunities for income beyond salary.
Just one fellowship that greatly benefits the teaching hospital allows the residency graduate to bypass what is needed to a place with better support, more team members, and less complexity along with higher salary and opportunities for income beyond salary.
The dollars flowing to these lower concentration places are too few to support the workforce - regardless of any training intervention. NO Training Intervention can help until payments are increased for generalist and general specialty services. Only then can more be hired and better supported along with the team members to address the massive and growing shortages.
Movement from 6% of health spending to 12% for primary care is required with nearly all of the additional dollars going to lower concentration counties - and without requirements for additional tasks that distract team members from restoring access.
Additional Funding Is Not Needed for Residency Positions
The last decades of residency expansion have been funded teaching hospitals and the
VA.
Once again the most lines of revenue and the top reimbursement in each line goes to teaching hospitals. They have demonstrated the ability to create and sustain residency positions.



Comments
Post a Comment